 Ever since I can remember I had excruciating painful periods and excessive bleeding. The cramping was so bad that I would take tons of ibuprofen just to get by. I was in misery every month. I was so afraid that I never went to the doctor. Of course, the writing was on the wall, but I did not want to accept it. I was in denial.
Ever since I can remember I had excruciating painful periods and excessive bleeding. The cramping was so bad that I would take tons of ibuprofen just to get by. I was in misery every month. I was so afraid that I never went to the doctor. Of course, the writing was on the wall, but I did not want to accept it. I was in denial.
In the fall of 2015, I had such bad cramping and excessive bleeding during my period that I could not take the pain anymore. I was 44 years old at the time and could also feel a lump in my groin area that was very large. I finally gave in and went to the gynecologist. She did an exam and by the look on her face, I knew that it was not good. She said that I had a very large fibroid. She told me that she felt that it was not cancerous and that she wanted to order an internal ultrasound. In the following days, I went for the internal ultrasound and it was confirmed that I had a non-cancerous fibroid and would need surgery.
I went into her office to discuss the surgery more. She wanted to make sure that I did not want any more children because after this surgery it would not be possible. I already had a child, and my husband and I had decided that we did not want any more children years prior. I also had to decide if I wanted to keep my ovaries or not. She suggested that I keep them so that it would not cause me to go into menopause immediately. She told me if they removed the ovaries, it would be very difficult at first to deal with side effects such as hot flashes, hormonal imbalance, and mood swings. I opted to keep them. She said that she hoped to be able to do a vaginal hysterectomy so long as the fibroid was small enough to do so. She had a photo on the wall and explained how the surgery would be performed. I would be put to sleep and then she would make small abdominal incisions aided by long, thin surgical instruments inserted through the incisions. The surgeon would then remove my uterus through an incision made in my vagina. The benefit of this was that I would have a much quicker recovery time since they would not need to make a huge incision in my lower abdomen. Additionally, I was told the surgery would end up making my hospital stay only 2-3 days. I agreed to the surgery and I was scheduled for the next week. She said that she could have done the surgery earlier, but I was taking so much ibuprofen for so long that she was worried about excessive bleeding. Leading up to the surgery, I could only take a pain killer that was Tylenol-based. I was in quite a bit of pain that week. I also asked if it mattered if I was having my period at the time and she said that it did not. Before I left that day, I had a date set for the surgery. I was told that I would be called the night before with an exact time to come to the hospital.
The night before surgery, I received a call and was told to be at the hospital at 6 am. I was not able to eat or drink after midnight. When I arrived with my husband, I was checked in at the desk and the nurse told me to come back with her. My husband had to remain in the waiting room. She told me that once I was prepped that she would come and get him to be with me. She escorted me to a very small room with curtains dividing it and she handed me a gown and a bag for my clothing. She told me to undress completely and put the gown on and that she would return in a few minutes. After undressing, she returned. She took my vitals, asked a series of questions, and inserted an IV. She then had my husband come back so that he could stay with me until surgery.
At 8 am, my surgeon came in and asked if I had any final questions. She reminded me that after this surgery, I would not be able to have children. A few minutes later, a transport person came in to take me to the operating room. The nurse escorted my husband to the waiting area and told him that they would call him to the desk when the surgery was over. I was then wheeled to a hallway outside of the operating room. There, the anesthesiologist came and explained that she would inject medication into my IV and that I would be put to sleep. After I was on the operating table, a tube was placed down my throat. The medication was injected in the hall and I do not remember anything after that. Please note that I have had surgeries since, and I was never put to sleep before going into the operating room.
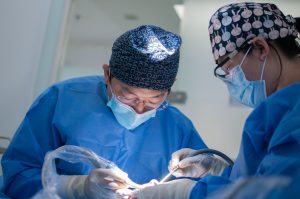
When I woke up in the recovery area I was in a lot of pain. The recovery area was a large room with curtains between patients. My nurse was handling two patients. She came over and tried to make me comfortable with IV medication, an ice pack, and heating pads. After my pain levels decreased, she invited my husband to come into the room and be with me. He explained that the surgery lasted nearly 6 hours. The surgeon had already spoken to him and had left for the evening but would come and see me the next morning. From what I gathered, when she went to do the surgery, the fibroid was so large that she did not feel comfortable doing it. She had to call in another surgeon and it took almost an hour for him to come in and take over. My fibroid was the size of a large orange. Also, at some point during the surgery, a catheter was placed so that I would not have to get up to use the bathroom for 24 hours following the surgery.
After several hours, I was taken to my room; my husband came with me as I was wheeled to my room. About 5 minutes after arriving while the nurse was checking my bandages and getting me comfortable, I had the most intense hot flash of my life. I was soaked from head to toe and felt as if I had a shower. I never expected this to be happening. Every time it happened, and my husband and the nurse would get me changed and dry, it would happen all over again. This was, in my opinion, the worst part of the entire thing. The nurse gave me ice packs that I would keep on the back of my neck and that really helped, but it was still tough.
I barely slept that night. The next morning the doctor came in and told me that pathology had come back, and I did not have cancer. Of course, I was thrilled but I knew that I would not be running any races anytime soon. She took the catheter out and I then had to go to the restroom multiple times in an hour. My husband helped me since I felt terrible calling the nurse so frequently to come and help. I still had the IV connected, so he had to be careful not to tangle it. The hot flashes continued, almost hourly. I was encouraged to walk the halls to keep moving. I had pretty bad pain all day and was given both oral and IV pain medications. I was able to eat three meals that day. When the doctor came back later on that day, she looked at me and said that she felt that I needed to stay another day and I agreed. I was afraid to go home since I knew that I was still getting IV pain medications.
The next morning, she came in and told me that I would be going home later that day. I was not to lift anything heavier than a gallon of milk for at least 6 weeks. I was still experiencing quite a bit of pain upon being released. I had 3 incisions in my abdomen, but these incisions had steri-strips and could be removed after 7 days. I was allowed to shower at this point but no baths or swimming. I would follow up in a week with a doctor’s appointment and was also not allowed to drive until she gave me the approval to do so.
When we arrived at home, I had to get to bed which was tough since our bedroom was upstairs. There was no way that I would be able to sleep on the couch. I did make it up that night, but it was very painful. I spent the next week in bed. My husband went to work at 3 am, and he would leave shelf-stable food in our room so that I was able to eat when he was gone and not have to go down the steps. I also found that propping myself up in bed was helpful as I could not sit in a chair or on a couch without pain. Ice packs were helpful, and I continued taking Oxycodone for about 4 or 5 days. I continued to have extreme hot flashes, but they did go away about 2 months after surgery.
A week later, I returned to the doctor. I felt that I was still in too much pain. She said that I would have a much longer recovery time due to the size of the fibroid that was removed. She also said that when she got the pathology information that I also had endometriosis. This accounted for all of the pain and misery that I had experienced over the past 25 years. She checked the incisions to make sure that they were healing well and told me to come back in 6 weeks. The steri-strips were removed at this appointment, and I was cleared to drive. She told me to wait for 6 weeks to have sexual intercourse.
For the next 2 months, I continued to recover. I had a very physical job at the time so I could only work a couple of hours each day until about the 6-week mark. At that point, I still did not lift heavy items for another 4 weeks. From what I understand, my recovery time took longer than most.
I was back to my normal routine 3 months after the surgery. However, one night, I was awoken by a sharp pain in my side that had me in tears. My husband was at work, so I had my son drive me to the hospital. If I called an ambulance, they would not have taken me to the hospital that I had the surgery at and I did not want that to happen. My husband met us at the hospital. I was diagnosed with a burst cyst of the ovaries. I wanted to bring this to your attention because I have had this happen 3 times since surgery. The pain when it is bursting is a 9 and you are toppled over in pain. My ovaries were the only things that were spared during my surgery. If I had to do it again, I still would have kept my ovaries because I feel that they have kept my hormones balanced.
The content of this article is for informational purposes only and is not intended to be a substitute for professional medical advice.




One Response
Thank you so much for sharing your story. I am going for the same surgery with the same symptoms on Thursday 9/8/22. I also have a large fibroid and other smaller ones in my uterus and another one in the cervix. I’m severely anemic due to the fibroids and have been taking weekly IV Iron infusions for the last 7 weeks and 2 blood transfusions the month prior. It’s been rough but I don’t give up that easy. Again thanks for helping me understand what is going to happen.
Keep fighting 💪
Rhonda